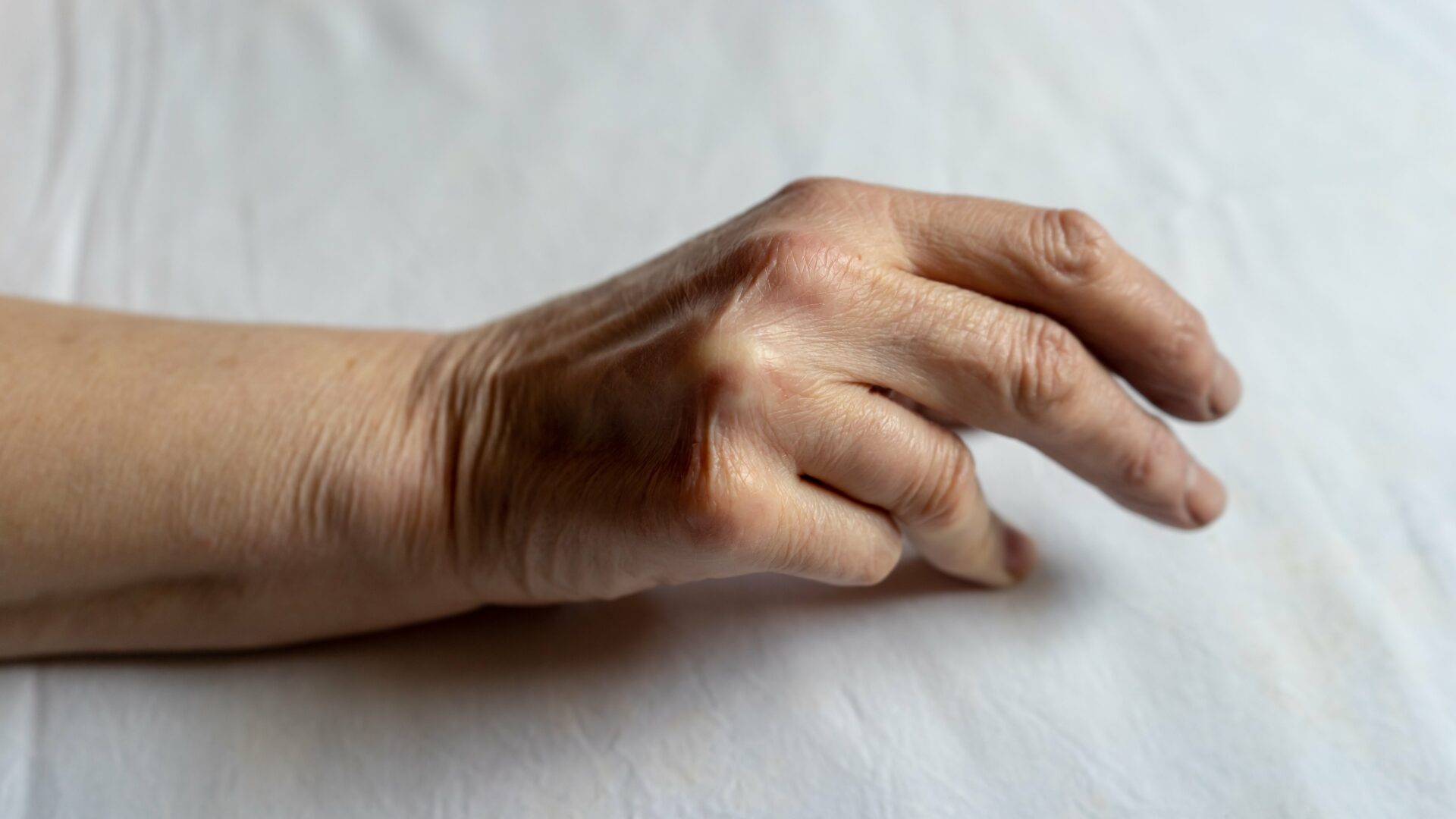
Dupuytren’s disease is a condition that affects the palm tissue. Later stages of the disease’s development can affect the fingers, and this is known as Dupuytren’s contracture.
The condition is also known to affect the knuckles, soles of the feet or penis. It is not life threatening, generally considered painless, and the cause is unknown. Despite that, there are plenty of queries that people have on a condition that affects a high percentage of the ageing population.
Below you can find answers to some of the frequently asked questions.
What is Dupuytren’s disease?
It arises due to a thickening of the connective tissue (fascia) in the palm of the hand. The tissue develops into nodules, which in turn thicken into cords that curve the affected fingers towards the palm.
The condition is benign (non-cancerous) and the early symptoms are commonly accepted as painless. Despite that, it is a progressive condition that deteriorates into a worse state over time. The eventual contraction of the affected fingers can produce mild pain. The most frequently affected fingers are the ring and baby fingers.
Once the condition develops, the affected fingers can’t be straightened completely. In this case the most routine of tasks can become problematic, even putting your hand in your pocket to take something out can be an issue.
Notable people to have suffered from the condition include the late British Prime Minister Margaret Thatcher, former President of the United States Ronald Reagan and Prince Joachim of Denmark. It goes to show just how common Dupuytren’s is.
Where does the name ‘Dupuytren’s Disease’ come from?
Baron Guillaume Dupuytren, a 19th century French surgeon, researched and described the disease in 1832. After dissecting a patient’s hand in his practice at Hôtel-Dieu in Paris, he diagnosed a thickening of the connective tissue as the cause of finger contractions. He was the first medic to do so. He went on to perform an operation in front of a live audience to solidify his claim of being the first to not only detect a cause for the condition, but suggest that it is treatable.

Baron Guillaume Dupuytren [Wellcome Images]
In the late 1700s, British doctor Henry Cline Sr. anatomically described the condition and suggested a surgical treatment for it. He was the first anatomist to determine that the disease was caused by the fascia as opposed to the tendons, a concept that was previously stated further back in history.
Both Dupuytren and Cline Sr. correctly connected the disease to the fascia, but Dupuytren was the first to approach it as treatable. So although it is unclear as to why the full credit has been given to Dupuytren, his claim can be wholly appreciated.
How does Dupuytren’s disease develop?
Most common cases of Dupuytren’s disease begin with the formation of miniscule lump(s) under the skin of the palm. These are called nodules, they bed themselves into the connective tissue (fascia.) Most cases will see the nodules fail to develop beyond this stage, but they will remain under the skin of the palm as a symptom of the disease and can grow up to around one centimetre in width. If you fold your hand, you will notice a natural crease or wrinkle that sets in your palm. Nodules most commonly develop along that line, near the ring and pinky fingers (of course, they do develop in other areas of the palm as well.) Although generally painless, they can be slightly tender in the early stages of their development.
The nodules will continue to thicken and condense into tight bands. These are called cords. If the chord runs up a thumb or finger, they will gradually draw the affected fingers downward so that they curl toward the palm. Most commonly affected is the ring finger, this is followed by the little, middle, and index fingers. Occasional cases of Dupuytren’s disease see the thumb affected. The maturation of the cords can bring around feelings of inflammation, tension and pressure as the joints begin to stiffen into the curvature. Approximately 25% of people who develop nodules will go on to develop cords and experience Dupuytren’s contracture.
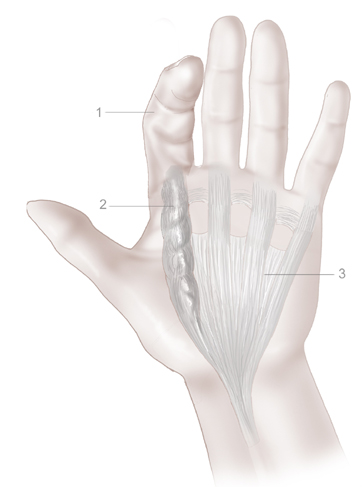
1. Contracted index finger, 2. Nodules in the palmar fascia, 3. Unaffected connective tissue [Taken from the NHS website.]
What are the causes of Dupuytren’s disease?
The exact origin behind Dupuytren’s disease is currently unknown. At present, we can only look to genetic factors and medicinal history to produce a detailed account of who may be at risk as opposed to why Dupuytren’s may develop for them.
Who is most likely to get Dupuytren’s disease?
Heredities appear to be the greatest influence for Dupuytren’s disease, and the NHS highlight that 4 to 7/10 people who have developed Dupuytren’s have at least one elder relative who also suffered from it. The condition is thought to be autosomal dominant. What does that mean? You only need to be passed the condition-causing gene by one of your two parents, because it is not an X or Y chromosome.
Connected conditions such as Ledderhose or dorsal nodules are also known to increase Dupuytren’s risk.
There are strong demographic trends that point to a sharp rise in Dupuytren’s cases for men over the age of 50, especially those of northern European historical descent – further evidence that there are genetic factors at play.
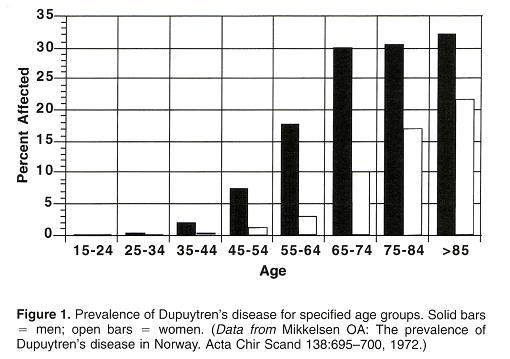
In Norway, you can see that the percentage of the population affected by Dupuytren’s increases sharply with age. [Figure taken from dupuytren-online.co.uk]
What are the risk factors of Dupuytren’s disease?
As discussed above, age, sex and descent are all non-modifiable risk factors that could put someone further at risk of contracting Dupuytren’s disease. Further to those, there are also one or two modifiable factors that extend the danger.
According to this study, alcohol use can be aligned with an increased risk in Dupuytren’s disease. It concluded that regular, prolonged exposure to alcohol is indeed associated with a higher contracture risk. It considered how alcohol affects the human metabolism through its interaction with the liver.
Smoking has a damaging affect on red blood cells and their ability to carry oxygen around the body. A decreased oxygen supply to the hand can lead to an increased risk of Dupuyten’s disease, therefore.
How is Dupuytren’s disease treated?
Unfortunately, there is no known cure for the condition. There are plenty of treatment options available, though. They are generally available when the disease begins to seriously affect hand function, to a point where one is unable to carry out daily tasks.
The majority of Dupuytren’s cases are mild, yet some of these will still require a form of non-invasive treatment to ease the situation.
Non Surgical
The most typical form of non-surgical treatment is a needle fasciotomy. Firstly, the palm is numbed with a local anaesthetic, followed by the insertion of a needle into the chord that has formed in the fascia. The needle acts to split the chord, releasing tension, and ultimately reducing the contracture. The benefits of needle fasciotomy, other than a reduction in contracture, also include a faster recovery time in comparison to open surgery and a suitability to the elderly demographic who can’t withstand invasive surgery.
Ladan Hajipour conducts needle fasciotomy treatments at her clinics.
The purpose of radiation therapy is to stop the need for invasive surgery by pointing controlled doses of x-ray radiation at the nodules and cords in the palm and fingers. The aim is to disrupt the growth of the benign cancerous tissue. Patients should be made aware of the risk, albeit a miniscule one, that radiation therapy carries with regards to cancer.
Collagnase is a medicine that can be injected into chords that have formed in the palm. The medicine acts to soften the cords over a 24 hour period, after which a doctor can then straighten out the bent finger(s) to bring back a range of movement in the affected digits. There are side effects to this, which include inflammation and itching. Ladan Hajipour does not currently offer collagnase treatment.
Surgical
Open fasciotomies can be implemented to work on more severe cases of Dupuytren’s. The procedure is carried out under local anaesthetic, and involves a surgeon making an incision into the palm to cut the connective cord tissue, easing the straightening of the fingers. Although the recovery time is naturally longer than the non-invasive treatment options, the result is generally very positive and patients can regain full use of their hand. Other surgical treatments include open, regional, segmental and dermofasciectomies and you can read about them here.
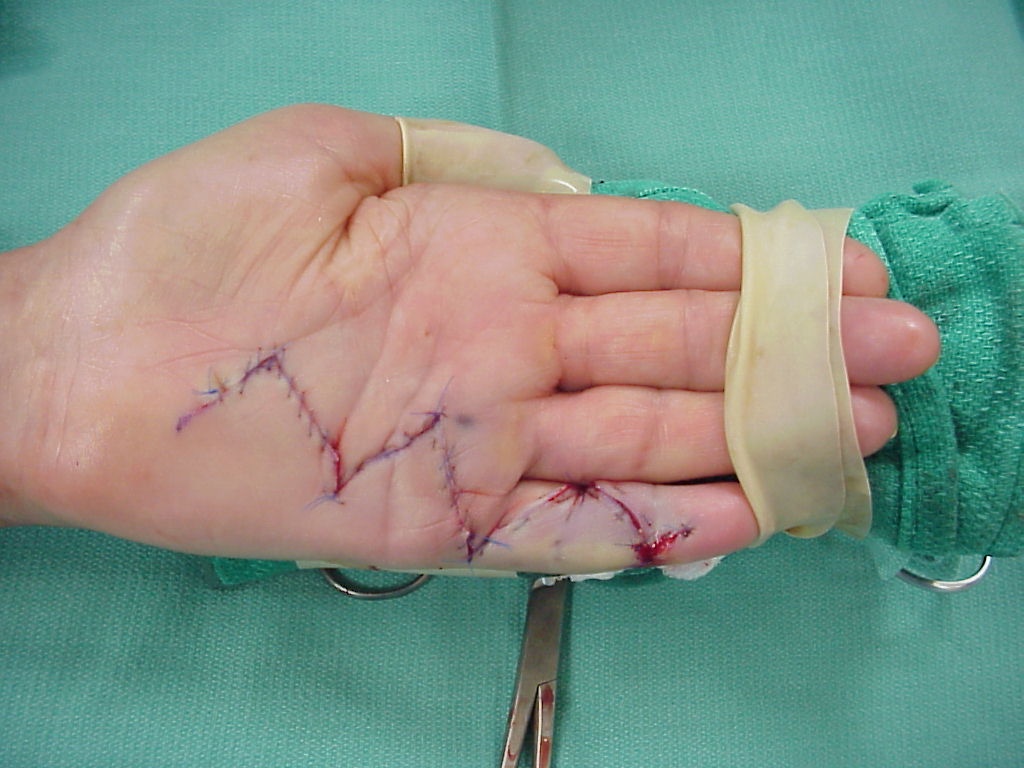
A palm after Dupuytren’s surgery. [Image credit goes to eatonhand.com]
How do I know when I need treatment for Dupuytren’s disease?
Treatment will only be considered if the condition has developed to a point where the fingers have started to contract, although special circumstances include pain or loss of function as a result of the nodules in the palm.
Simply put, the majority of those with Dupuytren’s will not require any treatment. For most cases of the condition, symptoms will never develop beyond a mild stage. A thickening of the palmar fascia is generally nominal enough to live with. History shows that a high percentage of cases have failed to develop into serious contracture. So, GPs generally do not refer you to a specialist unless you struggle to straighten your hand onto a flat surface.
Remember, there is no cure. Any treatment you are given is in the interest of bringing your symptoms to a manageable level.
How can I avoid Dupuytren’s disease?
The general consensus is that there is no fool-proof Dupuytren’s prevention technique. This is because the condition is known to be hereditary, people are born with the genes that trigger the disease.
Although inconclusive, researchers have reason to believe that the palmar fascia can become more sensitive to environmental risk factors such as liver disease and diabetes if the genes are present. From this perspective, it appears wise to limit ones personal lifestyle to lessen the negative potential that these risk factors have.
Read more about Dupuytren’s disease here.